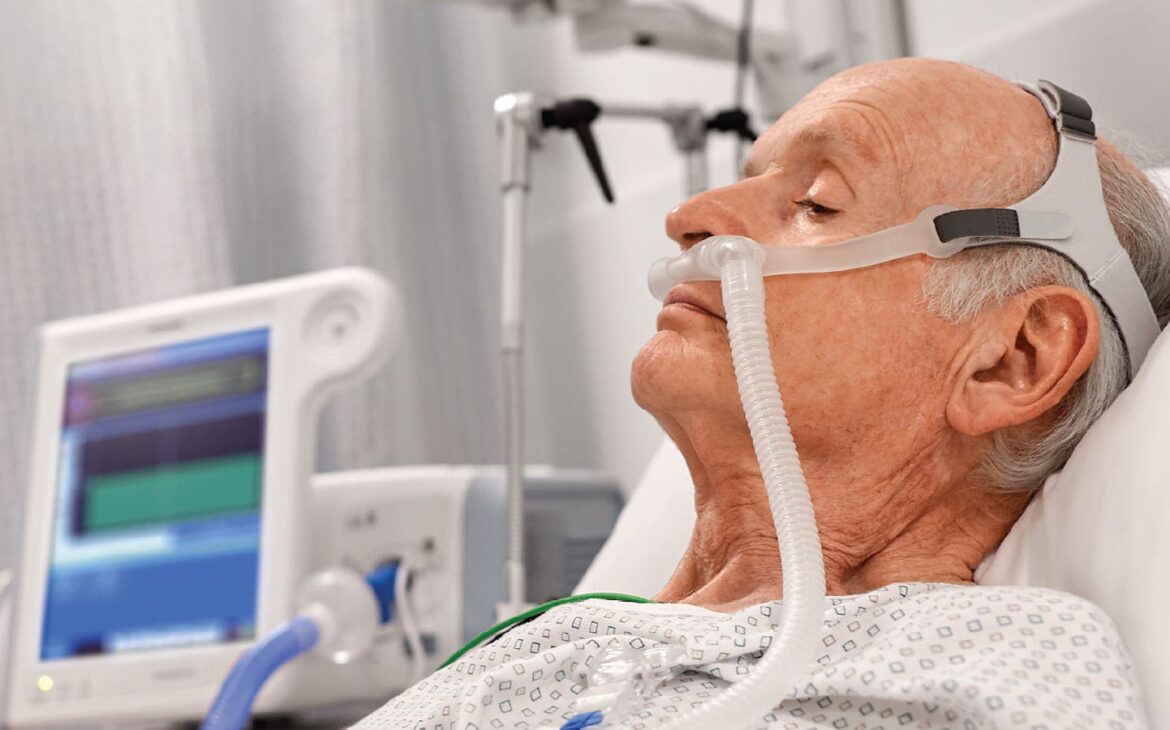
- A randomized trial examines two types of oxygen therapy in severe cases
By Molly Walker, Deputy Editor-in-Chief, MedPage Today
The use of high-flow oxygen was associated with a lower need for mechanical ventilation and a shorter recovery time compared to conventional oxygen therapy in patients with severe COVID-19, according to a randomized trial conducted in Colombia.
Thirty-four percent of patients randomly assigned to receive high-flow oxygen via nasal cannula were intubated by day 28, compared with 51% of those randomly assigned to conventional oxygen therapy (HR 0.62; 95% CI: 0.39-0.96; P=0.03), reported Gustavo Ospina-Tascón, MD, PhD, of the Valle del Lili Foundation in Colombia, and colleagues in JAMA
Time to clinical recovery was only 11 days for patients in the high-flow oxygen group versus 14 days for the conventional oxygen group
"The data suggest that high-flow oxygen therapy may decrease the need for endotracheal intubation and the risk of therapy intensification in patients with acute hypoxemic respiratory failure, but with no apparent effect on mortality rates," the authors wrote.
Although most international guidelines recommend high-flow oxygen therapy to treat patients with severe COVID, "the evidence to support it is very limited," they noted.
The High Flow Nasal Cannula in Severe COVID-19 with Acute Hypoxemic Respiratory Failure (HiFLo-Covid) study was an open-label randomized trial that examined patients in three hospitals in Colombia from August 2020 to January 2021. Adult patients with suspected or confirmed COVID-19 infection, respiratory distress, and "an arterial partial pressure of oxygen to fraction of inspired oxygen ratio less than 200 due to COVID-19" were included.
The co-primary outcomes were the need for intubation and the time to clinical recovery up to day 28.
In total, 220 patients were randomly assigned, 109 to high flow oxygen therapy and 111 to conventional oxygen therapy, and 199 patients were included in the analysis (mean age 60 years, 32.7% women).
Clinical recovery occurred in 78% of patients in the high-flow oxygen group and in 71% of those in the conventional oxygen group.
Patients in the high-flow oxygen group had a shorter median number of ventilator-free days, but with a wide confidence interval (28 vs. 24 days; adjusted OR 0.77; 95% CI: 0.33–1.68). The need for renal replacement therapy and the length of hospital and ICU stay were similar between the groups, and the hazard ratio for death on day 28 was 0.49 in the high-flow oxygen therapy group compared with the conventional oxygen therapy group.
In addition to conserving resources, the use of non-invasive ventilation for COVID patients could "prevent complications related to invasive mechanical ventilation, sedation, delirium, and neuromuscular paralysis," Ospina-Tascón and his team wrote.
Limitations of the data include the lack of double-blinding, due to the open-label nature of the trial, the lack of generalizability of the results, as the patients came from only three hospitals in one country, and that co-primary endpoints could increase the potential for type 1 error.