August 20, 2019 by the University of Liverpool
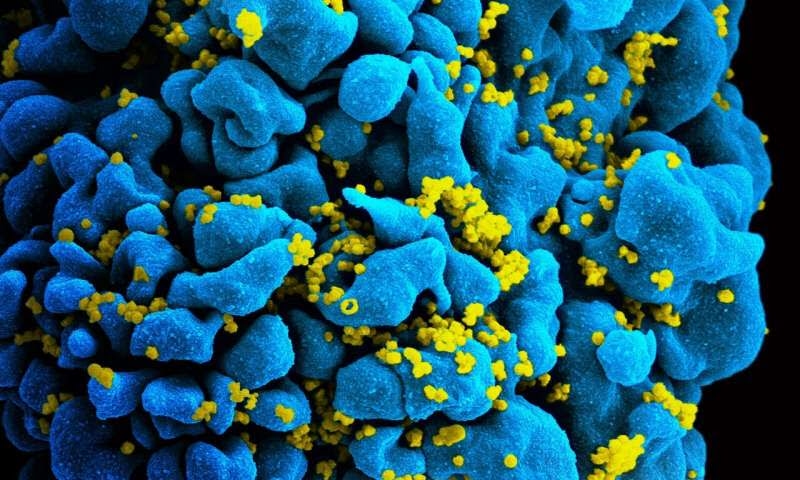
Scanning electron micrograph of an HIV-infected T cell. Credit: NIAID
Researchers from the University of Liverpool and Queen's University Belfast have received more than £1 million from the Engineering and Physical Sciences Research Council (ESPRC) to examine the use of nano-engineered microarray patches (MAPs) to improve the delivery of long-acting HIV drugs.
HIV/AIDS remains a major public health threat, with an estimated 36.9 million people living with HIV worldwide in 2017. That same year, HIV-related illnesses claimed nearly 1 million lives globally, and 1.8 million people were newly infected. During 2017, approximately 21.7 million people gained access to antiretroviral therapy, representing 59 percent of adults and 52 percent of children living with HIV.
In 2016, 42 percent of diagnoses occurred at a late stage of infection, and HIV awareness is declining in the UK, highlighting the value of preventative treatments. Current methods for administering medication for HIV treatment and prevention are far from optimal and require a strong commitment to daily tablet intake.
This project is led by Professor Ryan Donnelly from the Faculty of Pharmacy at Queen's University Belfast. Collaborators from the University of Liverpool include Dr. Marco Siccardi and Professor Andrew Owen from the Department of Molecular and Clinical Pharmacology, and Professor Steve Rannard from the Department of Chemistry.
The research is based on formulation technology from the University of Liverpool, licensed by Tandem Nano Ltd, a recent spin-off company from the University of Liverpool. It will design and test a new type of transdermal patch with hundreds of tiny projections on its surface, called microneedles. After painless application to the skin, these microneedles will dissolve, releasing drug nanoparticles for the treatment or prevention of HIV. These nanoparticles will dissolve over weeks or months, so patients no longer need to strictly adhere to oral regimens.
The research will leverage world-leading expertise in long-acting drug delivery from Liverpool and Belfast, and utilizes advanced computer-based pharmacokinetic models, bespoke nanoparticle manufacturing processes, and an exciting new approach to MAP formation.
Dr. Marco Siccardi said: “The technology being developed here is unique and could revolutionize the treatment and prevention of HIV infection. It offers the opportunity to improve HIV drug delivery, simplifying the management of HIV therapies in the future. We will use state-of-the-art expertise, including high-powered computational models, to design and predict the behavior of MAPs, accelerate product design, and inform laboratory experiments.”
Professor Andrew Owen said: “Recent global developments in long-acting drugs promise to change the paradigm of chronic disease therapy. We continue to strive to harness technological advances to improve patient outcomes, while balancing innovation with the need for broad availability worldwide. This project encompasses three of the University of Liverpool’s priority research areas and is nestled within a growing portfolio of local activities in the delivery of long-acting medicines.”
Professor Steve Rannard said: “This new program with Queen’s University Belfast is a further extension of the nanomedicine activities in Liverpool that began in 2009. Our collaborations include Africa, Europe, the UK and the US, and the partnership with Professor Ryan Donnelly in Belfast is an excellent opportunity to develop our research into new delivery routes that may have future ramifications beyond HIV.”
Professor Ryan Donnelly commented: “At Queen’s University Belfast, we are delighted to be collaborating with our colleagues in Liverpool on this pioneering work program. We have always been committed to developing truly patient-centered interventions, and therefore, the exploitation of our MAP technology for the prevention and treatment of HIV/AIDS is of particular importance.”
Provided by the University of Liverpool
From: https://medicalxpress.com/news/2019-08-nano-engineered-microneedles-hiv-drug-delivery.html