As monkeypox continues to spread in Europe and North America, primarily among gay and bisexual men, much remains to be learned about its impact on people living with HIV or at risk of contracting it. So far, it appears that people receiving antiretroviral treatment with well-controlled HIV do not experience worse outcomes.
In the United States, the Centers for Disease Control and Prevention (CDC) reported 72 confirmed cases of monkeypox in 17 states and Washington, D.C., as of June 14, including 15 cases in California and New York. Worldwide, the World Health Organization (WHO) has confirmed 1,285 cases in more than two dozen countries where the virus is not endemic as of June 10. The United Kingdom, Spain, Portugal, Germany, and Canada have reported the majority of cases outside of Africa.
Monkeypox Basics
Monkeypox virus is transmitted from animals and from person to person through close contact. This can include skin-to-skin contact, kissing, and contact with contaminated clothing or bedding. It can also be transmitted through respiratory droplets over short distances, but it does not spread over longer distances like the coronavirus that causes COVID-19. It is not known whether monkeypox is sexually transmitted in semen or vaginal fluid, but it can be spread through contact with sores during sexual intercourse.
While anyone can contract monkeypox through close personal contact, most of those affected by the outbreak in non-endemic countries are gay, bisexual, and other men who have sex with men. Many of them reported recent international travel, and many visited saunas or attended large events, including a Pride festival in the Canary Islands.
Monkeypox, which is related to smallpox but less severe, typically causes flu-like symptoms, swollen lymph nodes, and a rash that can appear on the face, mouth, or anywhere else on the body. In the current outbreak, many men have developed lesions on their genitals or anal area. The lesions can resemble chickenpox or common sexually transmitted infections (STIs) such as herpes or syphilis. Monkeypox has an incubation period of up to three weeks before symptoms begin, and the illness usually lasts two to four weeks.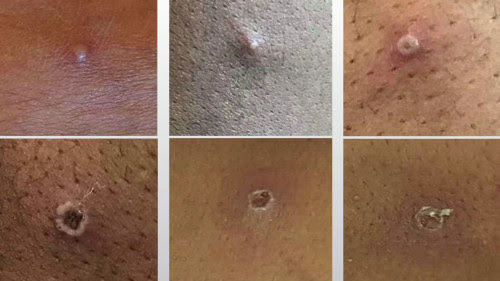
Monkeypox lesions, UK Health Safety Agency
Most people with monkeypox recover without treatment, and so far, there have been no confirmed deaths in the current outbreak. But the sores can leave scars, and people with more severe illness can develop complications. Severe outcomes are more common among children, pregnant women, and people with weakened immune systems. Vaccines and antiviral medications used to prevent and treat smallpox are also effective against monkeypox.
Monkeypox and HIV
There is a lack of data on monkeypox among people with HIV. Previous studies in Africa found that people with uncontrolled HIV had worse outcomes, including larger and longer-lasting lesions, more complications, and several deaths, but people with well-controlled HIV appear to have better outcomes.
“There is limited data among people living with HIV, but those taking antiretrovirals and having a robust immune system have not reported a more severe course,” according to the WHO. “People living with HIV who are not on treatment or remain immunocompromised may have a more severe course, as documented in the literature.”
“Currently, we do not recommend any specific action for people with HIV beyond monitoring clinical presentations and exposure history,” the British HIV Association said in a statement. However, the organization suggests that people with a CD4 count below 200, a persistently detectable viral load, or a recent HIV-related illness should be considered at higher risk.
In the United States, Demetre Daskalakis, director of the CDC's Division of HIV/AIDS Prevention, declined to say whether anyone diagnosed with monkeypox is HIV-positive, citing patient confidentiality concerns. The CDC has not yet issued guidance on monkeypox for people living with HIV or at risk of contracting it.
In Europe, a recent Eurosurveillance report described four cases of monkeypox among gay men in Italy. Two were HIV-positive and receiving antiretroviral therapy, and two were HIV-negative and receiving PrEP. Three had attended the Canary Islands event, and one reported traveling for sex work. All reported unprotected sex with different male partners while traveling. All reported lesions on various parts of the body, including the genitals in three cases and the anal region in two. Three had very low levels of monkeypox virus DNA in their semen. All recovered without treatment.
Another report in the same issue described 96 cases of monkeypox in Portugal, with more detailed information on a subset of 27 cases. All were men, mostly in their twenties or thirties. Fourteen were HIV-positive. Most reported recent sex with multiple partners, and several had visited saunas. Six had genital ulcers and five had anal ulcers.
The UK Health Security Agency (UKHSA) has published the most detailed information to date on monkeypox among gay and bisexual men in the current outbreak. As described in a recent technical report, epidemiologists interviewed 45 men diagnosed with monkeypox who had known or suspected links to transmission through gay sex networks up to May 25.
Nearly all reported sex with other men, and 20 reported group sex, during the monkeypox incubation period; 20 reported more than 10 sexual partners in the past three months. In addition, 20 men reported visiting on-premises sex venues, such as saunas, darkrooms, or sex clubs, in the UK or abroad. Approximately a quarter reported having sex in other cities or with people who are not UK residents.
Most of the men (27) had been diagnosed with an STI within the previous year, but the majority (32) were HIV-negative. All the men living with HIV were receiving antiretroviral therapy, and over 90% had an undetectable viral load. Of the 32 HIV-negative men, 29 were linked to sexual health services for HIV pre-exposure prophylaxis (PrEP).
Be aware, seek care
Epidemiologists don't know how long monkeypox has been circulating in Europe and North America, and they're not sure if it has spread beyond the social and sexual networks of men who have sex with men.
Many gay and bisexual men routinely monitor their sexual health and seek medical attention if they experience unusual symptoms, but cases may be missed in less vigilant populations. Because many men at risk for monkeypox have connections to sexual health clinics, these can be good settings to offer education, testing, vaccination, and treatment. Sex venues and Pride events are also potential settings for targeted interventions.
While acknowledging the need to direct education and resources to the most affected communities, experts and advocates emphasize that monkeypox is not a “gay disease”—anyone can contract it through close personal contact—and many fear that associating it with gay men could trigger the same kind of stigma surrounding HIV.
“Stigma distorts science,” Daskalakis said during a recent monkeypox forum organized by InterPride. “Monkeypox can potentially affect everyone, but we need culturally appropriate information to reach the networks that are experiencing increased transmission right now. Pride is a great way to spread messages; we’ve been using it for decades to disseminate information about HIV and STIs.”
Experts urge anyone who develops symptoms suggestive of monkeypox, and particularly gay and bisexual men, to seek medical attention and get tested. Remember that the rash can be subtle, with only a few lesions and no flu-like symptoms.
Testing and contact tracing are key strategies for containing disease outbreaks, but testing for monkeypox is currently limited. About 70 state labs can test for orthopox (the virus family that includes smallpox and monkeypox), but a monkeypox diagnosis must be confirmed by the CDC. Some advocates are calling for more widespread testing, for example, at STI testing clinics and at community venues and events.
People diagnosed with monkeypox are urged to cooperate with contact tracing efforts, but, as the UKHSA report points out, this can be difficult when people have sex with casual or anonymous partners. Tracing all contacts found at large gatherings is also a challenge.
People with monkeypox should isolate themselves and avoid close contact, including sex, for three weeks. Cover the sores with clothing or bandages. Wash clothes, towels, and bedding in hot water, and disinfect surfaces that come into contact with the sores. Although it is unclear whether the virus is transmitted in semen, the UKHSA recommends using condoms for eight weeks as a precaution. Monkeypox is contagious until the sores have completely healed and the scabs have fallen off.
People who believe they may have been exposed to monkeypox should monitor themselves for three weeks, the maximum duration of the incubation period; ideally, they should avoid sexual intercourse and other close contact during that time.
Some basic precautions can help prevent the spread of monkeypox. If you feel sick, avoid close contact, including sex, and public gatherings. In crowded settings where skin-to-skin contact cannot be avoided, long sleeves and long pants reduce exposure. Wash your hands frequently. Avoid sharing sex toys and personal items such as toothbrushes. Because the virus can be transmitted through respiratory droplets during face-to-face contact, a well-fitting mask can help prevent transmission. However, the virus is not airborne over longer distances, such as during casual conversation or while passing someone in a grocery store, according to the CDC.
Monkeypox can be contained through ring vaccination or targeted vaccination of close contacts. The United States maintains a large stockpile of an older smallpox vaccine (ACAM2000), but this can cause side effects, especially in people with compromised immune systems or skin conditions. A safer, non-replicating vaccine (Jynneos, also known as Imvanex and Imvamune) was approved in 2019, but it is currently in short supply. Several countries are using this strategy for high-risk personal contacts and healthcare workers. The province of Quebec in Canada offers the vaccine to men who have had sex with two or more men in the past two weeks. However, experts do not recommend vaccination for the general population.
With Pride season in full swing, most experts and advocates are not recommending canceling events or closing venues where people have close contact, including during sex. But some are urging LGBTQ organizations to do more to spread the word.
I believe the #LGBTQ community needs to step up its game now against the monkeypox. We have the opportunity to contain this outbreak in our community, but we must act quickly, decisively, and put all our resources into this task.
“Everyone needs to step up their game. This is a moment of total engagement,” tweeted veteran HIV activist Gregg Gonsalves, now an associate professor at the Yale School of Public Health. “We have an opportunity to contain this outbreak in our community, but we must act quickly, decisively, and put all our resources into this task.”
From: https://www.poz.com/article/monkeypox-people-living-risk-hiv-need-know

