The World Health Organization (WHO) has ended the global health emergency for xenophobia, marking the end of a 10-month juggling act by the UN health agency as it struggled to cope with concurrent global pandemics.
The announcement comes just days after the WHO declared the end of the global health emergency for COVID-19 last Friday, three years and 6.9 million lives after the virus rose to a global pandemic in January 2020.
At a press conference at WHO headquarters in Geneva on Thursday, Director-General Dr. Tedros Adhanom Ghebreyesus said that despite the change in designation, both viruses still pose "major health challenges."
“While the COVID-19 and polio emergencies are over, the threat of resurgence waves remains for both,” Tedros said. “Both viruses continue to circulate and both continue to kill. This does not mean the work is finished.”
What now?
Tedros's announcement follows a recommendation from the WHO's emergency committee on the pandemic, discussed in a lengthy closed-door meeting on Wednesday. The committee assessed that the virus no longer constituted a public health emergency of international concern and recommended ending the emergency declaration.
The leaders of the emergency committee emphasized that the end of the emergency is not the end of the fight against the virus, but the beginning of a policy change.
“Removing the Public Health Emergency of International Concern in no way means that mpox is no longer an infectious disease threat,” said Dr. Nicola Low, vice-chair of the mpox committee that issued the recommendation. “[It] means moving towards a strategy that will manage the long-term health risks posed by mpox rather than the emergency measures that are inherent in public health emergencies.”
The committee's recommendations include integrating mpox into national pandemic prevention, preparedness and surveillance programs, as well as into existing sexual health services for diseases such as HIV.
“It is vitally important that we continue the efforts that have already begun,” said Dr. Rosamund Lewis, technical lead for mpox in the WHO health emergencies program. “As long as the virus is given the opportunity to continue spreading from person to person, it also has the opportunity to evolve.”
The affected communities are key to sustained success.

A central element of the WHO mpox committee's policy recommendations is the emphasis on continued engagement with affected communities, such as men who have sex with men.
Outside of endemic African countries, men who have sex with men account for almost all mpox cases, including 99% in the United States. Meanwhile, about half of all mpox infections have occurred in people living with HIV.
Immunocompromised patients with HIV not only have a higher risk of severe mpox disease, but they also present an ideal environment for the virus to mutate and evolve to become more transmissible.
Including mpox as a standard in sexually transmitted disease monitoring, detection, and prevention programs will allow men already connected to sexual health services to be screened for mpox at the same time as other STIs, streamlining surveillance and treatment for both patients and health authorities, experts said.
“Typically, around half of the cases have been among people living with HIV. Gay and bisexual men who have sex with men are the most affected population group here,” said Andy Seale, WHO senior advisor on global HIV, hepatitis, and sexually transmitted infections programs. “Outbreaks like this begin and end in communities, and it is these communities that will help us stay on top of surveillance, intelligence, and dynamics as the outbreak continues to evolve.”
WHO experts also credited community organizations for their key role in helping to contain the virus outbreak through education, awareness, treatment and vaccination campaigns.
“We are now seeing steady progress in controlling the outbreak based on lessons learned from HIV and by working closely with the most affected communities,” said Tedros. “The work of community organizations alongside public health authorities has been critical.”
Endemic African countries are another story
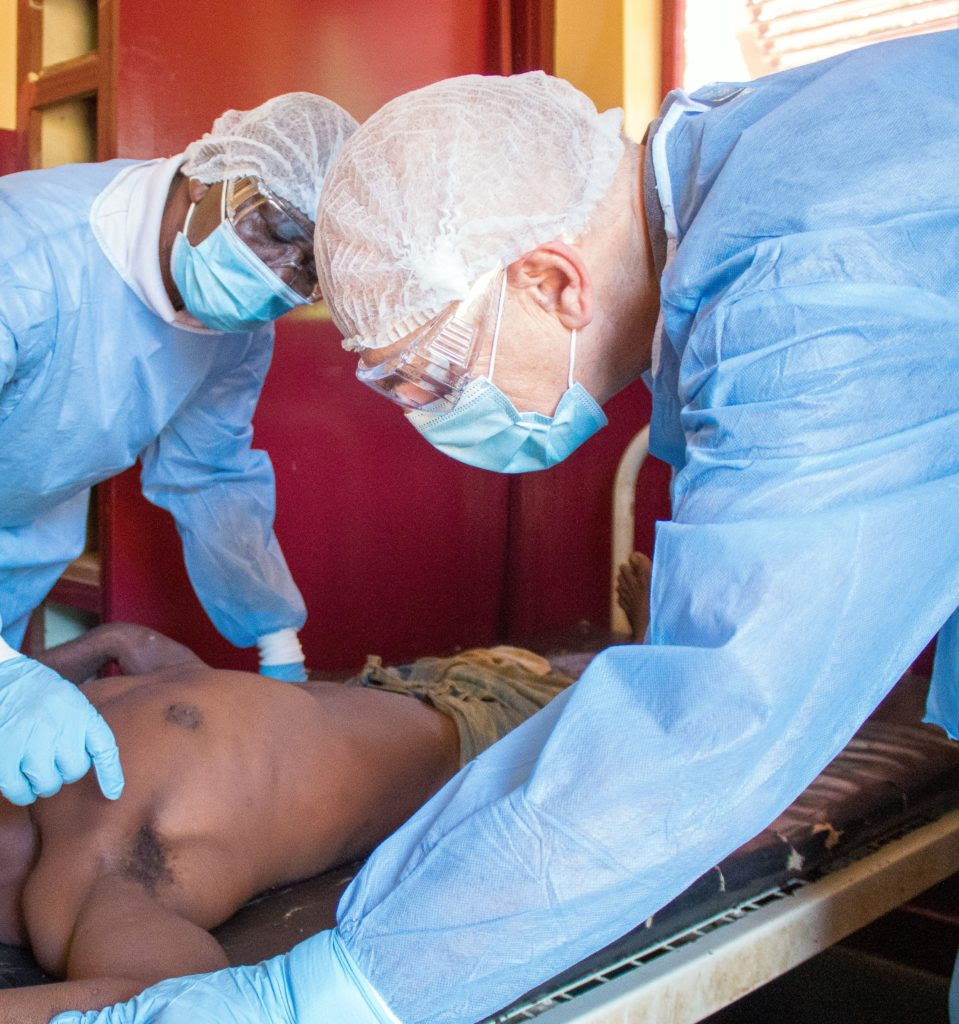
While a smallpox vaccine manufactured by the Danish company Bavarian Nordic was rapidly deployed under emergency authorizations in the United States and Europe at the start of the mpox emergency, the manufacturer's monopoly on the vaccine patent and limited stocks before the global outbreak made access difficult, even for wealthy countries.
“[We recognize] that there have been fewer commitments than expected or less than desired with respect to vaccine equity and distribution, particularly in Africa,” Lowe said.
"But it is also recognized that we still do not have enough evidence on the effectiveness of the vaccine from randomized controlled trials."
Currently, the WHO recommends the use of the Bavarian Nordic vaccine primarily for post-exposure prophylaxis and only for prevention in specific circumstances.
Lowe said that randomized controlled trials are being planned to improve data on the vaccine's effectiveness in endemic countries.
Another obstacle to eradicating mpox is the mystery of how the strain of the virus evolved to spread globally and maintain prolonged person-to-person transmission.
Until that question can be answered, the road to ridding the world of the virus remains long.
"How it went from a possible zoonotic source to the human population with amplification of transmission is something we still don't have information about," Lewis said.
“We need to continue supporting the countries and regions where this research into the origins of the virus is underway, which will be fundamental to our understanding in the future.
“African countries were dealing with mpox long before this outbreak began, and they will continue to deal with it for some time,” Lewis said.