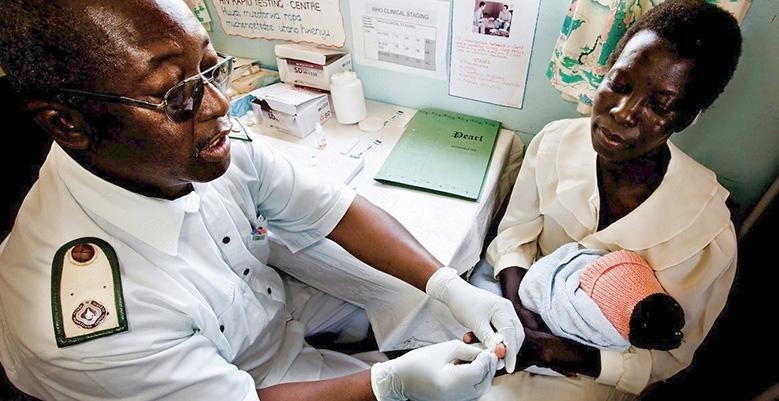
The World Health Organization's new policy indicates that countries should replace immunoblotting and linear immunoassays, which can only be performed in laboratories, with simpler methods, such as rapid diagnostic tests.
The international health organization, which launched the new HIV testing policy in late November, made the recommendation following compelling evidence that rapid diagnostic tests (RDTs) and enzyme immunoassays (EIAs) produce faster and more accurate results than laboratory methods. These newer testing strategies also cost less because they are less complex and can be performed by healthcare workers with varying levels of training and experience, rather than specialists.
Because Western line and transfer immunoassays can only be performed in laboratories, health centers have to send blood samples for analysis. This leads to delays in informing people about their HIV status and, for those who test positive, can also delay the start of treatment.
A systematic review commissioned by the WHO found that immunoblotting and linear immunoassays also result in a higher number of indeterminate diagnoses than newer testing strategies, meaning that people must be retested. This not only causes uncertainty for the individual, but if this request is not heeded, the opportunity for diagnosis is lost.
The evidence review found that nearly half of all indeterminate results generated by laboratory methods related to people living with HIV are outdated. This means that a significant proportion of HIV-positive individuals experience delays in starting treatment due to these obsolete diagnostic methods, which is not only detrimental to their health but also increases the likelihood of subsequent transmission.
In stark contrast, RDTs and EIAs allow people to know their status in a much shorter timeframe, meaning they can start treatment more quickly if they are HIV-positive. The relative immediacy of these newer methods also means that people who test HIV-positive but are considered to be at high risk of infection can be linked to PrEP immediately instead of having to wait.
Because non-specialized personnel can perform RDT or EIA, HIV testing using these methods can be carried out in community settings and health centers. This means that people from criminalized groups who may be afraid to use clinics despite being at higher risk of HIV infection, those who cannot afford the costs associated with clinic visits, and people who are reluctant to access public testing services due to stigma may be more likely to get tested.
Although most countries have already adopted rapid diagnostic tests (RDTs), some still use Western blot and line immunoassays to confirm HIV infection. This is common in several Western European countries, as well as in parts of Eastern Europe, Asia, and the Pacific. For these countries, switching to more efficient testing methods will initially require additional time and resources, but will have a greater impact and reduce costs in the long run. The WHO policy brief contains a technical checklist of things countries in this position should consider when making the switch, such as the need to retrain laboratory staff to take on supervisory and quality control roles.
Photo credit: DFID / CC.
From: https://www.avert.org/news/who-urges-countries-switch-laboratory-based-hiv-diagnostics-point-care-testing